government
Some states limit Medicaid fees for certain ED visits
■ Emergency physicians say some exclusions could discourage patients with potentially serious conditions from seeking timely care.
By Doug Trapp — Posted Oct. 17, 2011
- WITH THIS STORY:
- » Relatively few nonurgent ED visits
- » Related content
Washington -- Nearly all states have at least one program to encourage Medicaid enrollees to reduce emergency department use considered unnecessary. But at least a few have begun limiting Medicaid fees for what they classify as inappropriate visits.
Medicaid managed care plans in 43 states have programs to reduce inappropriate emergency department use. This is the most prevalent special quality initiative by Medicaid MCOs, said the authors of a 50-state survey of Medicaid managed care organizations released Sept. 13 by the Kaiser Family Foundation. Most of the programs are not controversial.
But a few states -- such as Iowa, Tennessee and Washington -- are limiting Medicaid emergency department pay for conditions the states deem nonemergent. Program administrators say they are prioritizing state Medicaid spending for the most urgent patients -- not patients who visit EDs for nonemergencies dozens of times annually.
Emergency physicians are bristling at the new restrictions. They say patients can't know in advance if a chest pain is a sign of a heart attack or something less serious.
"Sometimes as doctors we don't know. That's why we keep you for 24 hours and do tests," said Leigh Vinocur, MD, spokeswoman for the American College of Emergency Physicians. Its Washington chapter is suing over its state's limits.
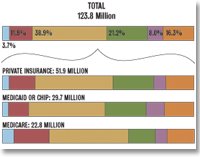
Medicaid enrollees are the most frequent ED visitors per capita. They visit EDs about twice as often as uninsured people and Medicare beneficiaries, who in turn visit about twice as often as the privately insured, according to the Centers for Disease Control and Prevention.
Many Medicaid enrollees rely on health centers for primary care, but some do not feel as if they have a primary care physician, said Malika Fair, MD, an emergency physician at Prince Georges Hospital in Cheverly, Md. The hospital cares for many Medicaid enrollees. Dr. Fair said she doesn't blame them for coming to the hospital. "I don't think that people misuse the ER," she said. "Everyone thinks they have an emergency."
Limits bring a lawsuit
On Oct. 1, Washington state implemented an annual limit of three visits per Medicaid enrollee for a list of 700 conditions and diagnoses the state declared nonemergent. The state won't pay for nonemergent care, beginning with the fourth annual visit. The change is fulfilling a legislative mandate to reduce Medicaid ED spending by at least $70 million over two years.
The state also is addressing high ED use by limiting frequent visitors to one physician and one pharmacy, arranging case managers to get patients into primary care, and making grants to hospitals for community planning for nonemergent care, said state Medicaid agency spokesman Jim Stevenson.
Washington Medicaid administrators are trying to reduce ED visits for the estimated 3% of Medicaid enrollees who seek drugs at hospitals or have recurring mental health issues, said Jeffery Thompson, MD, MPH, chief medical officer for Washington's Medicaid program. Some Medicaid enrollees visit EDs more than 100 times a year.
The list of 700 nonemergent conditions Washington implemented includes less serious problems such as warts and sore throats. But it also excludes payment for patients with chest and abdominal pain and breathing difficulties, which can be symptoms of serious illnesses.
The Washington chapter of the American College of Emergency Physicians agreed to a smaller list of 200 nonemergent conditions but rejected the final state list. "This list of nonemergent diagnoses puts patients in danger and unfairly targets the poor and those in most need of care," said Stephen Anderson, MD, president of the Washington ACEP chapter.
In response, the chapter on Sept. 30 sued to reverse the state's Medicaid ED visit limits. Other medical societies also oppose the limits. They say the state's decision could erode the prudent layperson standard in federal law, which requires plans to cover visits to EDs if they are based on a person's reasonable belief that he or she may be having a medical emergency due to symptoms being experienced, not based on a final diagnosis.
"It is unfortunate that it has become necessary to take legal action to protect Medicaid patients in our state," said Doug Myers, MD, president of the Washington State Medical Assn. "Physicians have been trying to work with the state for many months to fix these errors."
Fights in other states
Other states have imposed similar Medicaid ED limits.
Iowa's Medicaid agency on Sept. 1 began tiered payment reductions involving Medicaid ED patients without a condition the state says it will cover as an emergency. The agency reduced Medicaid fees to 75%, half or zero of normal rates for nonemergent ED hospital visits depending on whether the patient has a physician referral and is part of a state primary care case management program. The limits do not apply to enrollees who are younger than 21, pregnant, receiving family planning or who are admitted to the hospital.
"The rationale is to save public dollars and to discourage improper use of emergency rooms," said Roger Munns, spokesman for the Iowa Dept. of Human Services.
Tennessee ended Medicaid pay for 51 nonemergent conditions on July 1 as part of a budget reduction plan, said Kelly Gunderson, spokeswoman for TennCare, the state's Medicaid agency. The state's Medicaid program closely monitors access to care and requires all enrollees to sign up with a managed care plan and choose a primary care physician, she said.