profession
Disaster medicine dilemmas examined
■ Mass disasters require quick decisions about treatment that can lead doctors to question whether they made the best medical and ethical choices.
- WITH THIS STORY:
- » When duty calls, most -- but not all -- would answer
- » External links
Kansas City, Mo. -- Thirty years after the disaster, Joseph F. Waeckerle, MD, still prays that he made the right calls.
The 1981 collapse of the interior skywalk system in the Hyatt Regency in Kansas City killed 114 people and injured 216 under the crushing weight of concrete and steel. Dr. Waeckerle directed the rescue effort and decided with just a few moments' review who could be rescued and who could be offered only a morphine drip and advised to make peace with God.

Dr. Waeckerle
Dr. Waeckerle and others at the scene had to determine how to save the most lives and limbs with little assurance that their judgments would be well-regarded in the aftermath.
A medical disaster is when the need for care outstrips the available resources -- medicines, equipment, personnel. Such a chasm between demand and supply stretches far beyond a hectic day in the emergency department and requires a shift in ethical thinking because not every patient can get the care he or she would be entitled to under normal circumstances.
Which patients get the highest priority? What obligation do physicians have to respond to patient need in disasters? What should physicians do to prepare?

Dr. Pou
Definitive answers are hard to come by, but asking these questions in advance can help prepare the profession and public for the gut-wrenching decisions made in the heat of the moment. In December 2011, Dr. Waeckerle and a group of other physicians, nurses, bioethicists and disaster-planning experts gathered in Kansas City for a conference hosted by the Center for Practical Bioethics, a local think tank, to examine ethical dilemmas that arise when disasters strike.
The need for such discussion is pressing. In 2011, damages exceeded the billion-dollar mark for 12 weather and climate disasters in the U.S., breaking the record of nine disasters set in 2008. Natural disasters killed more than 1,000 people in 2011, the National Weather Service said. The trend is likely to worsen, climatologists predict. Terrorism and pandemic influenza, while not grabbing headlines as often as they once did, still loom as threats.
Applying ethical standards
The biggest challenge that disasters pose for doctors is that they require adjusting to a new reality about what care can be delivered. That mental shift is tough, said Griffin Trotter, MD, PhD.

Edens
"Doctors have a difficult time making a transition to a public health orientation where they have to focus on the bigger picture," said Dr. Trotter, an emergency physician and professor for the Albert Gnaegi Center for Health Care Ethics at St. Louis University. "We're used to seeing one patient at a time, and each patient deserves my complete attention and all the efforts I can possibly provide, and I'm going to do that before I move on to the next one."
There are some broadly accepted disaster-medicine triage principles, but how they are applied can differ greatly depending on the circumstances of the disaster. State laws governing public health powers in disasters also vary widely, as do the standards that apply to physicians during declared disasters.
In 2009, the Institute of Medicine issued guidance to states on establishing "crisis standards of care" in anticipation of a pandemic flu and a shortage of ventilators and other medical supplies. Only a handful of states have moved to integrate the standards into disaster planning, and a follow-up report from the IOM is pending. Also uncertain are the medical liability protections that apply for physicians who travel to other states to do disaster work.
Physicians can head off ethical conflicts by familiarizing themselves with the disaster-planning procedures, public health powers and care protocols in their area. Continuing medical education courses available from the National Disaster Life Support Foundation, supported in part by the American Medical Association, can teach physicians skills on how to respond when calamities strike.
Katrina a test of readiness
Anna M. Pou, MD, faced a legal ordeal after she weathered four days of stifling heat and 15-foot floodwaters to provide care to patients trapped by Hurricane Katrina at Memorial Medical Center in New Orleans.
Nearly 2,000 people in the hospital suffered with little water and no electricity as the stench of human waste burned the throat with every breath. Dr. Pou and two nurses were accused of killing four patients at the hospital with sedatives. The grand jury that heard evidence in the case chose not to indict. Dr. Pou said she provided appropriate palliative care to critically ill patients.
Dr. Pou, an otolaryngologist, said she and her colleagues felt ill-equipped to deal with the complex catastrophe embodied by post-Katrina New Orleans. "We were grossly unprepared. The drill we did was for a bus crash, not a hurricane," she said. "We need hands-on ethics drills."
Effectively cut off from the outside world, the doctors and nurses at Memorial devised a triage system to determine which patients would be rescued by helicopter or boat. They decided to send less critically ill patients first, believing those patients were likelier to survive a treacherous trip up a dark stairwell to the roof for helicopter rescue.
Benefits of disaster drills
Nurse Terri Edens said drilling for calamity made possible the quick evacuation of the 372-bed St. John's Regional Medical Center in Joplin, Mo., when the hospital was struck by an EF-5 tornado May 22, 2011.
"I've been a nurse for 30 years and have been actively involved in disaster drills," she said. "And until May 22, I was not a great proponent of disaster drills. I thought, 'You are disrupting my day.' And I thought that when disaster came, I'd panic anyway and forget everything I learned. But the knowledge does stay there. That's the only way I can explain that 117 people that day in the hospital worked as an organized, cohesive unit to evacuate a building with only one working stairwell."
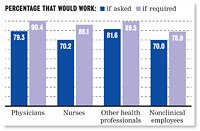
Another ethical challenge for physicians is how to respond to a disaster that poses great risks to themselves or their families. A nationwide survey of 526 doctors published in the September-October 2003 Health Affairs found that 80% of respondents were willing to treat patients in the event of a bioterrorist incident. However, 60% said they were unwilling to put themselves at risk of contracting a deadly, unknown illness to save others' lives.
The AMA policy says "individual physicians have an obligation to provide urgent medical care during disasters ... even in the face of greater-than-usual risks to their own safety, health or life." Medical educators should work to instill a sense of professional obligation to answer the call of duty in disasters, experts said.
For Dr. Waeckerle, an emergency physician, the decision to respond to the Hyatt skywalk collapse back in 1981 was not a hard one, but the life-or-death choices he faced still preoccupy him. He remembers telling one man pinned amid the skywalk wreckage that, to survive, he needed to have his legs amputated. The patient hesitated, and by the time the man agreed to the amputation it was too late to save his life.
"You make judgments. It's very easy for the people who are not there -- who've never been there -- to talk the talk when they have never walked the walk," said Dr. Waeckerle, former editor-in-chief of Annals of Emergency Medicine. "You always ask yourself every day for the rest of your life: Did I do the best I could for every person I took care of there?"
What's the answer?
"I hope so," he said.